Welcome to the UNC Chapel Hill School of Social Work Student Ambassador Blog! This blog was created by current student Ambassadors for people like you: prospective and new students interested in getting a glimpse of our Master of Social Work program from the student angle. Feel free to contact Student Ambassadors if you want to learn more!
Welcome to the Student Ambassador Blog!
Get Involved with the Student Health Action Coalition (SHAC)!
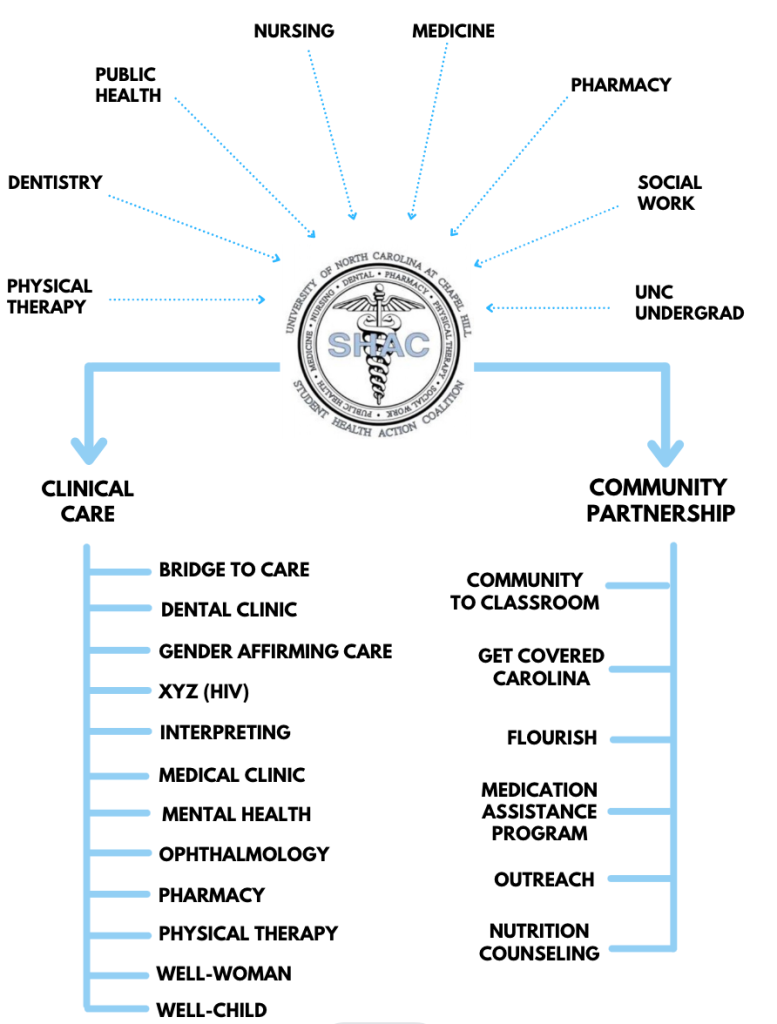
If you’re looking for a way to get involved during your time at UNC, as well as gain incredible experience caring for uninsured/underinsured patients within our very own community, join SHAC! The Student Health Action Coalition (SHAC) provides free health care and services to underserved populations while engaging UNC Health Science students in interdisciplinary service-learning activities.
SHAC’s Mission:
- Provide free health services to our uninsured and underinsured neighbors in Carrboro, Chapel Hill and Durham.
- Partner with communities to develop and implement sustainable programs.
- Create an interdisciplinary service learning environment for students in the Health Science programs at UNC.
SHAC’s Participation: SHAC is run entirely by student volunteers from many schools within UNC-CH including:
- School of Medicine
- School of Nursing
- School of Pharmacy
- School of Dentistry
- School of Public Health
- School of Social Work
- School of Business
- Division of Physical Therapy (Department of Allied Health Sciences)
- Division of Occupational Therapy (Department of Allied Health Sciences)
- Division of Speech and Language Pathology (Department of Allied Health Sciences)
SHAC meets every Wednesday night and if you’re looking for a chance to practice the skills you’re learning in the classroom and practicum I highly recommend joining SHAC! I am a Social Needs Navigator (SSN) and we enter the patient’s room after they have been seen by the medical team. We assess the need for assistance with housing, food, rent, utilities, transportation, while ensuring the patients feel safe where they live. We provide referrals to dental care and mental health counseling and create follow-up plans for each patient, ensuring they feel supported every step of the way! I have grown immensely since joining SHAC and am so thankful to pour into the community alongside other students!
Free Gaza
This morning, I listened to a story about 7 humanitarian aid workers who were killed in Gaza as they were delivering more than 100 tons of food aid to displaced Palestinians. The workers were from World Central Kitchen, many of whom were foreigners volunteering amidst recent chaos. Organizers of the humanitarian aid mission ensured previous authorization of the aid transfer with the Israeli army prior to the incident, although such assurance did not matter in the end.
This story is devastating. It is devastating that we are living in a world where humans trying to provide essential aid and care are killed, while those who are dropping bombs and authorizing missles are protected. It is devastating that so many efforts to sustain anything reminiscent of a lifeline in Gaza are being thwarted to the most violent extreme.
Current figures place the loss of life in Gaza to at least and still counting 32,845 people. This does not include the over 75,300 people injured and 8,000 people missing. This does not include those killed in the West Bank, nor does it include those killed before October 7th, 2023.
In addition to the loss of life in Gaza, the destruction of any potential for livelihood grows slimmer by the day. More than half of the homes in Gaza are rubble. Almost 400 educational facilities have been destroyed, and only around 10 hospitals are partially functional. In addition, 83% of Gaza’s groundwells have been destroyed or deemed unfunctional. Access to medical care grows increasingly dire while starvation, thirst, and injury, and fatality are grossly exacerbated.
It is difficult not to feel powerless right now, but I do not believe in staying silent. I believe that Social Work should be informed by social justice, ethics, and human rights, and that starts with social workers choosing not to be complicit or silent.
The UN defines genocide as follows:
“In the present Convention, genocide means any of the following acts committed with intent to destroy, in whole or in part, a national, ethnical, racial or religious group, as such:
- Killing members of the group;
- Causing serious bodily or mental harm to members of the group;
- Deliberately inflicting on the group conditions of life calculated to bring about its physical destruction in whole or in part;
- Imposing measures intended to prevent births within the group;
- Forcibly transferring children of the group to another group.”
All five of these acts have been committed and are happening right now. Most of Gaza has been leveled, including hospitals, schools, churches, mosques, residential spaces, and refugee camps. Entire generations of Palestinians have been murdered in one strike, leaving family members and children completely orphaned. The most vulnerable in Gaza, including children, pregnant folks, disabled folks, and the elderly, have little to no refuge or relief.
Social work students, institutions, and organizations should not only be ensuring the transparency and record of these atrocities, but should be doing everything they can to elevate the call for lasting humanitarian relief in Gaza. Palestinians deserve a right to live, just as we do here.
If you are interested in learning more about actions, organizing, or would like to have a conversation, please reach out to me: shareen@live.unc.edu
A Conversation with Clinical Assistant Professor Jaylen Cates, MSW
Levels of Care in the Mental Health World
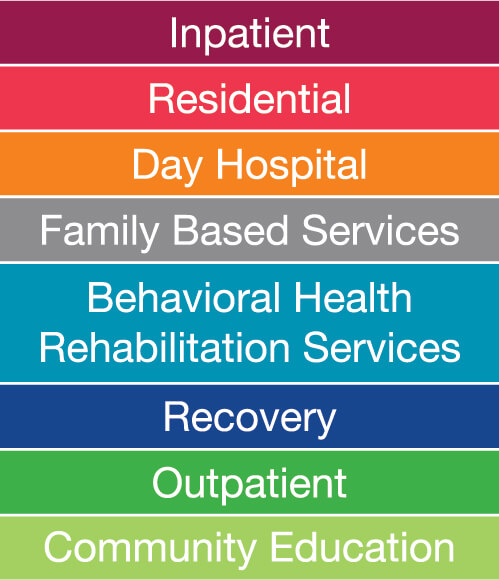
A common challenge for many clients is navigating the mental health industry, especially after they themselves, or a family member has recently been in a state of crisis. To better understand the differences in levels of care, as well as potential practicum placement options for you, here is a breakdown on different treatment types, ranging from the least to most intensive. As levels of care get higher, differences will become apparent in terms of the level of involvement and stream of information you receive throughout the week.
A general thought within the behavioral health workforce is that treatment is the most effective in the least restrictive environment. As a result, it is common for patients who do not meet admissions criteria at one level to have had a similar experience prior to that. While we can recognize the disparities and problems in our current mental health system, unfortunately, our patients are the ones who tend to suffer.
Outpatient Therapist
Duration: 1 to 2 times/week, for one hour
These sites often are your standard “therapy” sessions, where you can go for an hour and have that person in your lief over an extended period of time. UNC offers many placements at outpatient therapy facilities, including private practices, group practices, private pay companies, Medicaid-serving facilities, with a specific age group or population, etc. Additionally, these placements will often have you managing your own caseload of patients over the semester.
Intensive Outpatient Program (IOP)
Duration: 3 to 4 times/week, for 3 hours minimum
IOPs can range in terms of their duration, hours, and feasibilities. Many of these begin in the afternoon and continue into the evening. There are both individual and group IOP programs, so common tasks may include facilitating group therapy sessions, assisting with stepping up or down to a different level of care through case management, and providing individual therapy alongside these programs to participants outside of group hours.
Partial Hospitalization Program (PHP) / Day Hospital
Duration: 5 days/weel, for 6 hours minimum
PHPs are relatively new, and not well-known, even among the mental health workforce. These serve as day programs, meaning that participants have much higher safety concerns than those solely in individual or IOP programs. Additionally, they run during the day, meaning they require an order from an LCSW, Psychiatrist, Psychiatric Nurse Practitioner, etc., in order to justify insurance coverage, temporary withdrawals from work/school etc. Common tasks may include running weekly group therapy sessions, carrying your own caseload of clients, managing a cohort of patients who are together for an extended period every day, working on an interdisciplinary team, and helping implement behavioral changes in a group setting.
Residential Treatment
Duration: 7 days/week, often for the entire time of enrollment of 6-8 weeks minimum
Residential care involves patients who stay in a specialized facility to focus on intensive treatment. Although these are commonly associated with eating disorders, substance use disorders, and patients with externalizing behavioral symptoms, many programs exist that are more specifically geared to specific conditions and behaviors. These opportunities have a large clinical staff, so a variety of opportunities within these placements exist, where extensive collaboration can help provide a great overview of different responsibilities for the future.
Inpatient Settings
Duration: 48-72 hours of 24/7 care
Inpatient services, or a hospitalization, is the highest level of safety concerns. Here, patients are given a psychological evaluation and screening, where they receive constant monitoring for their safety. Common tasks in these settings may include administering these evaluations, discharge planning, brief therapy sessions with patients and family members, and again, working on an interdisciplinary team.
While I did not include every single level in depth, this graphic also includes opportunities that include early intervention efforts, which can be delivered in the community or in a school setting. Finally, you may here LOC being used, which also stands for Level of Care, and refers the assessment process to determine if a specific level of care is appropriate for that client.
Lessons Learned From My “Brand Yourself” Course
For my final semester, I enrolled in a half-semester course called “Brand Yourself” (GRAD725) which is taught in the Graduate School. The mission of this course is to prepare students for career development. I took this course because I wanted more structured support around my career-building goals. Last week was our final class meeting, and I am glad to say that the course was extremely valuable to me. Below are some major takeaways I think are useful for any person considering career development.
Resumes vs Curriculum Vitae (CV)
Here are some tips and suggestions related to creating and utilizing resumes and cv’s:
- A resume is usually a 1-2 page document that summarizes relevant work, educational, and/or volunteer experience, whereas a CV is typically longer. CVs have no page limit since they are supposed to include any and all relevant work/academic experience over the course of one’s career. It shocked me to learn that some people, such as the Dean of the Graduate School, have a CV of over 100 pages!
- Resumes are typically used for jobs related to industry (i.e. anything outside of academia), while CVs are specific to academia and research. For example, if I was applying to a research position at UNC, I would send my CV. If I was applying to the Department of Health and Human Services (DHHS), I would send my resume.
- It is important to tailor your resume to your job application.
- I used to have one resume for all things, but I learned that this is not always the best course of action when trying to be a competitive applicant. Especially since resumes already have limited space, it is important to pick and choose what to feature in the job you apply to based on what is most relevant (i.e. in terms of your skillset or experience).
The Importance of a Cover Letter
I did not realize how much a cover letter can elevate a job application. I learned that a lot of people tend to spend less time on their cover letters or don’t take the time to write one at all. Cover letters are an opportunity to convey direct intention about a position, and they can help applicants stand out if they are written well. One way to elevate a cover letter is to use the original job ad as a reference point (refer to “how to read a job ad” below). On the other hand, a poorly written cover letter or a cover letter that does not intentionally convey interest and relevant applicant experience can hinder one’s application.
Informational Interviewing
Informational interviews are a form of networking where you ask a person relevant questions about their career, position, organization, etc. to learn more about a job field or position. They are typically informal and can range anywhere from a few minutes to half an hour/an hour. You can also use informational interviews as a way to gain more information about a specific program or organization, such as insight into the quality of working with a specific organization.
Conducting informational interviews can be particularly beneficial for building new connections, being referred to relevant people in your network who you are not already connected with, and gaining insight into whatever work or role you are pursuing. Interviews can be as structured or unstructured as you feel is appropriate and can be done in casual conversation or in a more scheduled manner; they are designed to expand your network and understanding in a low-stakes way.
Reading Job Ads
Whenever I would read job ads, I would just skim through them in order to decide my interest and eligibility. I learned that this passive way of reviewing job ads on the front end was not serving me. Instead, I learned the value of actively reading a job ad, which means I now look for key terms (e.g. repeated terms) and use them to tailor my cover letter. For example, if I see a skill or task mentioned multiple times, I mark that word and use similar language in my application.
For Further Learning…
I hope that some of these takeaways and lessons are useful, as they have been incredibly insightful for me as I begin my journey into my career. It can be daunting to transition from being a student to entering the workforce, but there are numerous tools and supports designed to make this process smoother. After learning about them, I feel a lot less intimidated and a lot more empowered to take charge of my job search. If you found some of this information useful and would like access to more career tools, check out UNC’s University Career Services Website for more.
Finding Playful Rest in a World of Crisis
It’s impossible not to know about so much of the pain in the world of social work. Not that I want to be blind to it all, but how do I balance it while still living my best life and harboring hope? I don’t have a clear answer and I suspect it will be different for everyone. It’s also something I hope to be intentional about with others!
I want to practice living my life to the fullest no matter what that means on a given day. I want to laugh, play, rest, and nourish. I want to protect my mental health from the sea of information bombarding me 24/7 when I’m feeling too sensitive to cope. I want to have time to run through a forest and breathe the sweet air. There is so much goodness that is so easy to forget about.
Maybe I’ll always have that “I’M NOT DOING ENOUGH” fear swirling around in the background AND I think it’s important to remind myself that I’m here doing this major thing. To remind myself I have to take care of myself too so I can be of service. After everything I’ve lived through and overcome, I’m here and I’m trying. I also hold this for my peers as often as I can, because the truth is:
We care.
We are here.
We feel the pain of the world.
We feel the frustration of the broken systems.
And yet,
We are here.
We are doing something major.
We are trying.
But first,
We have to take care of ourselves.
It’s an easier-said-than-done kind of feeling, but so it goes with most mindfulness practices. That’s why we call them practices. I hope you’ll join me and others in being more intentional about this delicate balance when we can.
Battling Grad-itis: Wrapping up the Year Strong
It’s almost our time, Class of 2024! Being in this portion of the Spring semester can feel like a constant, never-ending Wednesday. I use this analogy because Wednesday is that in-between day where you know you’re close to the weekend, but you still have a little to go before getting there. For me, that is what the end of February and March feels like regarding graduation in May. In this period, it can be easy to get caught up in Grad-itis – the graduate school equivalent of high school senior-itis. I describe it as a feeling of knowing there’s an impending life transition, being ready to be finished with school, but finding it hard to get everything on the checklist done and power through. As I am learning how to move through this period, here are three tips I’ve picked up to help me stay successful while wrapping up the year.
- Write and schedule all commitments when you learn about them.
It can be super easy to lose track of responsibilities within this period, especially because there are so many factors to consider for our upcoming transition. We are being bombarded with questions about what life after graduation looks like, future occupations, trying to keep up with classes, staying committed to our internship, LCSW-A details (if that’s up your wheelhouse), among other life details. I have found it extremely helpful to write all responsibilities down in something you can easily reference to make some room in your brain and ensure all tasks are completed.
- Set aside a time to plan and review what you want to do after graduation.
If you’re anything like me, this has been the most challenging part. My mind is still trying to play catch up to the fact that graduation is approaching, so to plan for it feels like a big and daunting task. I have found it helpful to set aside a time in the future to look at job postings and requirements for the social work profession. I want to emphasize scheduling this time so you can mentally prepare for it as it approaches. If it still feels like too much to do as the scheduled time approaches, something I’ve found to ease anxiety is either 1) doing this process with a support person and/or 2) getting yourself a little treat or reward. Starting something is one of the most challenging steps in beginning a new experience, so having support in whatever capacity can be very beneficial. Once you complete the initial research, it can be much easier to follow up because now you have some idea of what life after graduation can look like.
- Indulge in and enjoy breaks and available time for yourself.
As important as making time for our responsibilities is, it is equally important to nurture space for ourselves. When we don’t take breaks and make time for the activities we enjoy, burnout can quickly and easily manifest in that space instead. It can be hard to do things you enjoy while you’re thinking about everything coming up, but try to keep in mind that while you’re in resting space, the responsibilities can’t and won’t reach you there. I have found it very helpful to stay organized during this time so that you know you’re not missing anything. We can get very caught up in trying to get all of our ducks in a row so that we can graduate, but this is also the time to rest before this significant transition so that we can be a bit more mentally centered for it. With that being said, don’t feel guilty for resting and taking care of yourself. If you don’t, it will be so much harder to take care of anything else.
This unique space before graduation is a period where a lot of life factors are taken into consideration. It can be easy to lean toward doing everything all at once or not wanting to do anything at all; I am here to tell you that wherever you fall on the spectrum, all of your feelings for this new experience are valid. Battling grad-itis can prove to be challenging, but I am confident we will all finish strong. We got to this point because of our excellent capabilities, which will propel us to succeed in the way that will be best for us. I’m sending positive energy and tons of support!
What is Good About it?
Amidst of all the uncertainties in life, when a bad thing happens, don’t forget to ask yourself “what is good about it?”
This is a piece of advice given to me by my mentor.
As an eldest daughter and a first-generation college graduate, I have been supporting my family financially since I graduated from my college. After 3 years of experience, I was leading a financial inclusion program at a social enterprise. I had a stable job with a high income; I was able to live together with my family; and I was able to support my family financially. I did have a dream to study abroad for my master’s degree, but I was not rushing or preparing to apply for my graduate school yet.
Unfortunately, in 2021, the military staged the coup in my country, Myanmar, and everything became hopeless in the country. The project I was leading was digital financial literacy program and moving towards the digital financial services. The military has control over the banking institutions in Myanmar and all the customers’ data were breached, resulting in the security risk to the customers who are involving in the revolution. People lost trust in financial institutions and even took their savings out of their bank accounts due to the potential bankruptcy risks. It became challenging to continue the program because people have security concerns to use financial services and the banking institutions lost credibility for their customers. Moreover, due to the double burden of Covid 19 and military coup, several companies in Myanmar are struggling just to survive. Many investors left the country and hundreds and thousands of people lost their jobs. I started having a concern about my own job security in the country. In addition to my career uncertainties, my well-being itself is a mess. I felt unsafe physically and emotionally. As someone who has witnessed directly or indirectly how the military killed people including children and youth, my safety is in danger as well. I could not stand near the window or on the balcony of my own house because I was worried about being shot. Even if I had to walk in the street or on the road, I constantly checked all the high buildings because I was concerned about the snipers and getting a head shot. I could not see my future either for my career or for my education or for my own safety – I felt stuck.
On the other hand, this feeling of being stuck pushed me to start implementing the dream of studying in a graduate school. I started looking into the scholarship programs for master’s degree. Still, I was helpless, and hopeless. I have been seeking professional help for my anxiety and the struggle I am experiencing. My mentor gave me an exercise to write down three things I am grateful for every day. In addition, he gave me one advice to ask myself “What is Good About it?” whenever something challenging (undesired or unwanted thing) happens in my life.
If there was no military coup and no other challenging conditions in the country, I may not decide to leave the country yet – my life trajectory would be different. The military coup, the uncertainties and security concerns in the country led me to decide to go for my long-lost dream of studying in graduate school and to take action to apply for scholarship. As a result, it has led me to receive the Fulbright scholarship and I was able to come to the US to study my MSW program at UNC Chapel Hill.
This whole experience helps me better understand my mentor’s words.
In life, things happen for a reason. Not all the things are good or bad. Everything has its own positive and negative sides. When we are in challenging situations, we tend to focus more on the negative sides of the situation.
Either good or bad emotions, we should have the ability to feel it; we should feel it; and we should allow ourselves to feel it because we are human. After that, we should try to see the positive side of the condition – even if there is only one that exist.
The National High School Ethics Bowl (and why social workers should attend!)

What is the National High School Ethics Bowl?
The National High School Ethics Bowl is hosted by UNC every year. It gathers more than 4,000 students across the nation in discussions around challenging moral issues. It differs from a normal debate model in that it allows students to collaborate with their opposing team to better understand the complexities of the case. They are rewarded for how respectfully they engage with their peers, the depth of their thoughts, and their ability to offer diverse perspectives on the issues at hand.
Why should social workers attend?
It is an incredible experience to watch these young people grapple with really complex moral dilemmas. As a social work student, who is also passionate about applied ethics, I participate as a judge each year because I love hearing their perspectives on real world issues. In the social work profession, we navigate many complex situations. I believe that volunteering at the bowl strengthens my practice!
Check out the cases!
The Pieces Come Together
The pieces come together-
This is the second month
of my second semester
of my final semester,
of a three year program.
In this second month,
of my second semester,
of my final semester,
of a three year program,
I have been relational.
Relating more deeply to what it means to be a dual-degree student, more relational with faculty/staff, more relational with the assignments required of me, more relational to any organization that I am a part of because
the pieces are coming together.
The pieces coming together do not attribute to me believing that I have every single step planned out beyond graduating.
The pieces coming together say I have contributed to my time in graduate school.
I am noticing and experiencing beautifully, diverse opportunities to effortlessly have my CV/Resume built.
I have skills to offer,
knowledge to lean into-
these pieces are coming together.
The pieces are coming together and it is because of the support of this program. The intention behind relationships here, the garnered support of my being.
This program invited every single part of me and because of the continued support of who I am-
the pieces are coming together.